15/01/2026
Strategy & Finance, News, Insights
20 years to build a hospital? How to save up to £7.5m by speeding up design and approvals for new hospitals & what this could mean for the New Hospital Programme
The PSC's analysis reveals that a substantial portion of this time, over 60%, is spent navigating the complex business case and approvals process.
What is the challenge?
Analysis by The PSC reveals it can take more than 17 years to build a hospital and often even longer from idea inception to sign off and build. For example, the Midlands Metropolitan University Hospital Strategic Outline Case (SOC) was approved in April 2004 but the construction is not yet finished (expected in 2024). Same observation for the Royal Sussex County Hospital (Brighton 3T’s) and the Moorfields Eye Hospital (Oriel), for which the SOC has been validated in 2008 and 2010 respectively, yet still awaiting delivery - originally they were expected in 2025 and 2027. This is an abnormal length of time relative to other buildings at similar cost and scale. Why is that?

Our research of schemes under the national New Hospitals Programme shows that more than 60% of the time spent is on business cases and approvals, often complicated by uncertain capital budgets and interruptions and changes of direction within national programmes.
These delays increase programme costs, lead to re-work and increase the risk that the “final product” is no longer relevant or meet the needs of a modern, digitally-enabled integrated health and care system.
The PSC’s research
We looked at the first eight hospitals to be built (Cohort 1) as part of the 40 planned under the NHP by 2030. For benchmarking purposes, we have looked at the elapsed time from when the Strategic Outline Case was approved to the actual delivery of the hospital. This means we haven’t included the often-significant work on some projects before the first approval. Therefore, the cost and time estimates may be underestimated here.
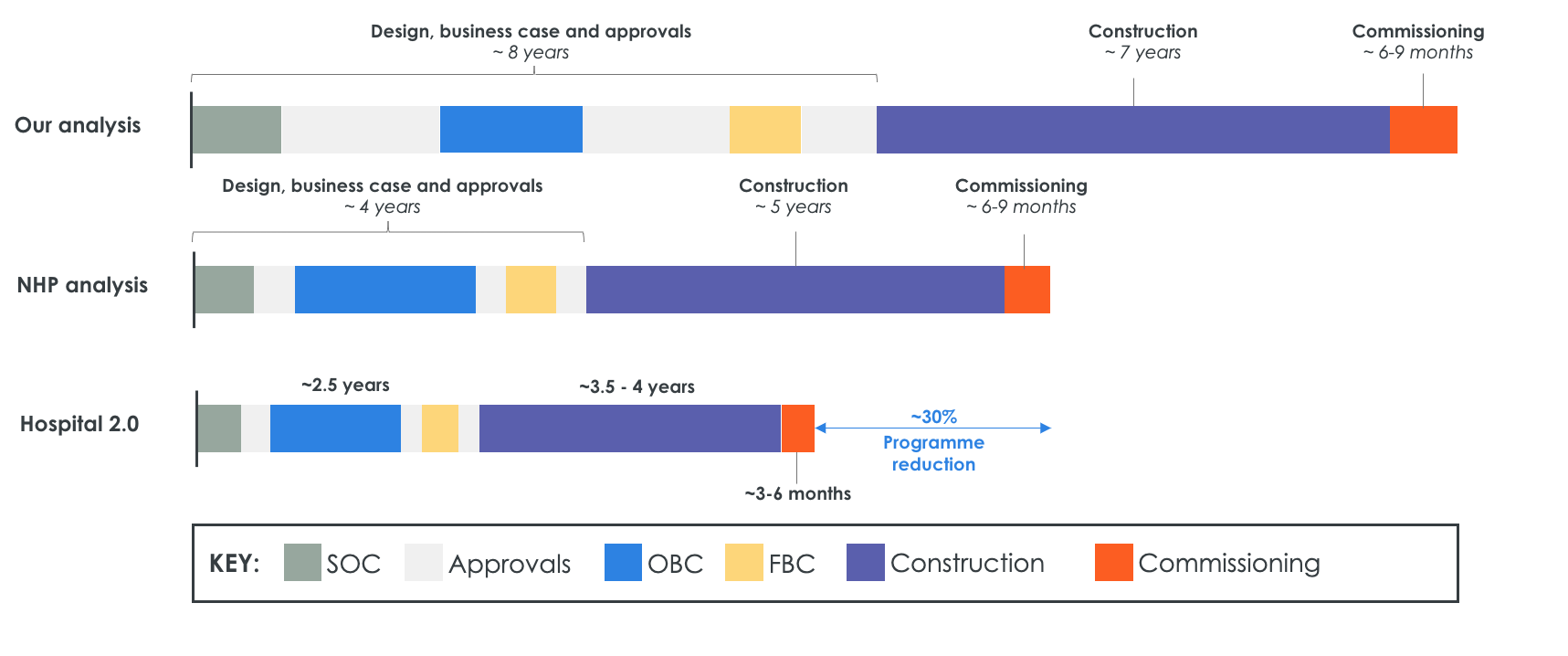
NHP’s own analysis appears to underestimate the pre-construction phase. Data shared in the Public Accounts Committee (September 2023) suggested a total timeframe of 11 years from end to end – 4 years for design, business case development and approvals and a further 5 years for construction.
How can it be explained?
Some challenges that schemes face are unique, but many are universal. Our research has highlighted that business case and approvals processes are particularly time-consuming.
This can be attributed to several factors.
First of all, the traditional lack of clarity on CDEL budgets mean programmes extend, waiting for budget allocation. Second, the decision-making process is hindered by extensive internal debate, and by the need to get support from various stakeholders across the system. Finally, the approvals process represents a considerable amount of time and resources, as it involves several parties (the NHP team, NHS England, DHSC and HM Treasury), numerous stages, and multiple requests for information that often need rework.
However, the NHP and delegated capital budgets to ICB’s provide a forward view of spend, which should enable more efficient planning and delivery.
Why does this matter?
Inefficiencies in the development and approval of business cases cost providers and health systems. We have estimated that Trusts can incur up to an additional £600k to £1m cost for every year of delay and rework in the approval process from programme spend alone. This lack of efficiency also means higher cost of assurance, as teams simultaneously spend a significant time and resources on the process. This excludes all other time (e.g. clinical time, Board time) that is not focused on the project and additional inflationary cost increases which have seen costs increase of 43% for cohort 1 and 2 hospitals between 2020 and 20231.
This can also adversely affect teams who have contributed to the project, detracting from the transformation possible and necessary before any future building opens.
Hospital 2.0 – standardization process
Hospital 2.0, which the national programme released in May 2024 is intended to not only standardise the design phase, but to set a new approach to streamline the whole end-to-end process, from the design to the construction to accelerate the building of the new hospitals. It seeks to reduce design, business case and approval time by 38%, as well as reduce construction time by up to 30%. With this approach, overall programme costs are expected to be reduced by 30%.
What can be done at national and trust level?
At both the national and trust level, steps should be taken to improve efficiency and reduce the time required to build hospitals.
At national level
The NHP team should:
- Provide a clearer timeline of future capital availability – to enable a greater transparency of approvals and timing and to allow the trusts to plan ahead and start developing the design and business cases when it is needed, thus preventing that their initiated work is left on shelf
- Streamline and speed up the approvals process – match resource and decision to forward looking timeline and clarify the review cycle: optimise review points, avoid multiple request and disproportionate amount of oversight, clarify roles and responsibilities (which national / regional team is responsible for reviewing what). This will require delegation of national budgets. Recent suggestions that NHP may adopt progressive and collaborative review between business case stages may help, so long as Trusts receive consistent advice throughout.
- Scale as appropriate – drive efficiency by introducing a set of standardised tools and templates that can be leveraged by organisations on a national or regional level, thereby avoiding replicating efforts for each organisation, but recognise local needs. Early indications are that this is beginning to happen, and the development of an NHP SOC Template is an important step – but the proof will be in how these meet the local needs
At trust level
NHS trusts should:
- Seek efficiency and adopt an agile approach to reach best answer at pace – arrange sprints with dedicated resources to produce business cases and secure internal alignment; meet needs of approval stage, not beyond, and align clinical, economic, financial, estates, digital workstreams to avoid errors and rework
- Clarify the governance – define and simplify the decision-making process and associated roles and responsibilities, ensure clinical input from whole system and set up to progress plans at pace across disciplines, not separate to them
- Seek integration – arrange regular discussion with local organisations (i.e., ICBs, local authorities, health authorities, clinical networks, etc.) ahead and during the programme, to anticipate local needs and ensure their understanding and relevance with other services outside the hospital
- Enhance quality and clinical engagement – obtain structured buy in and input from upskilled clinical teams, to strengthen and upgrade services’ quality through targeted change and transformation initiatives.
The PSC exists to make public services brilliant. We’re known for tackling the most complex challenges in the public sector, including an extensive track record in capital investment programmes. Get in touch with Jonathan Chappell at Jonathan.Chappell@thepsc.co.uk or Joe Cruden at Joe.Cruden@thepsc.co.uk to find out more about how we can support your organisation.
Latest News & Insights.

New report: The future of Smart Data – developing governance models
Commissioned by the Department for Business and Trade, our new report on…

Celebrating the value of lived experience involvement in public services: reflections from The PSC team
The PSC team share their thoughts on where they have seen the value and impact…
