Being believed
Our healthcare inequalities mini-series continues as we delve into why some patients from ethnic minorities aren't ‘believed’ and we consider some tried and tested approaches that could help patients be heard better.
Recent research about A&E attendees has highlighted the mixed experiences of patients in the emergency room. Many cannot commend NHS staff highly enough, but a small yet significant minority can leave feeling dismissed and ‘not listened to’.
Patients might attend repeatedly in the hopes of being better understood or treated, only for their repeat attendance to lead to the ‘frequent flyer’ label. This means that doubt is cast on the authenticity of their complaints, further reducing the likelihood of being fully heard.
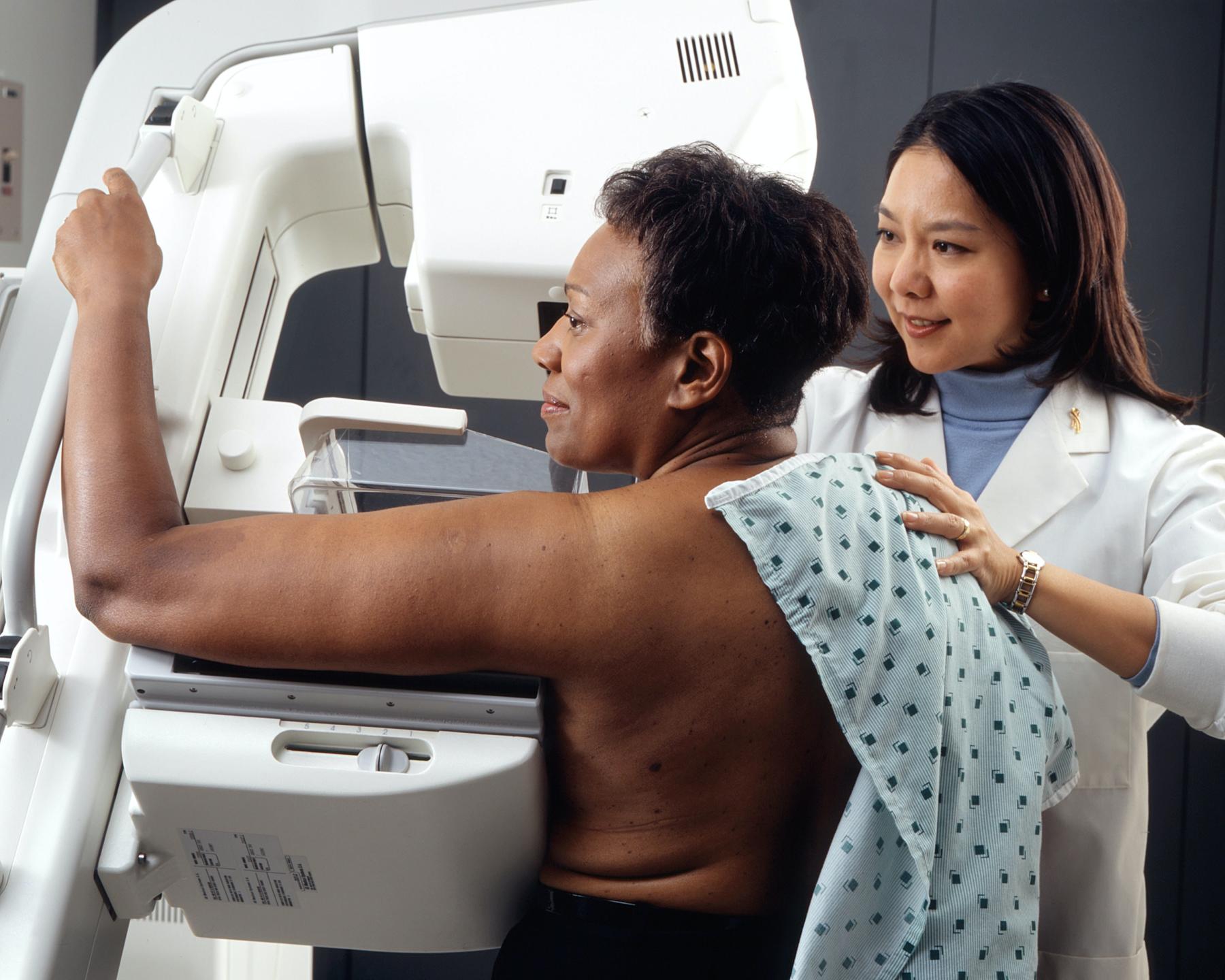
‘I had to go to ER for low potassium several times but all they say is to take potassium without even trying to figure out what is actually going on. I still don’t know the cause. It makes me super anxious to go because I’m scared to be labelled as a frequent flyer or to be flagged because I’m there too much’
- A patient complaint, online forum
Research suggests that those from BAME communities are among the most likely to be dismissed in healthcare settings. In the worst cases, these patients can end up missing out on crucial treatments.
Todd et al. (2000) found that black patients were significantly less likely than white patients to receive analgesics for certain fractures (57% vs. 74%), despite reporting similar levels of pain. A study of nearly one million children diagnosed with appendicitis revealed that black patients were less likely to receive pain medication (Kupperman et al. 2015). Black women are also five times more likely than white women to die as a result of complications in their pregnancy, in part due to this nefarious pattern of dismissing the pain of people of colour (MBRRACE UK, 2019).
At the root of these issues is systemic racism and the unconscious (and sometimes, conscious) bias that it can generate. The ways in which this manifests at the level of the patient and clinician is quite varied.
Let’s discuss medical training first. In our recent podcast episode ‘Skin deep: diversity in medical images’, paediatric registrar Dr Kaylita Chantiluke spoke about how lack of diversity in medical education can affect how clinicians interact with patients from diverse racial or ethnic groups. In short, if young medical trainees are not taught by a diverse group of professors or from materials generated by diverse authors, then they will be less likely to be able to understand how different diseases affect minority groups of patients. You can listen to the full conversation on Apple Podcasts and Spotify.
However, other, more deep-lying and insidious historical notions around race also affect this. For example, a study revealed that 63% of the white medical students surveyed agreed with the statement that ‘black people have thicker skin than white people’, and 22% believed that ‘black people had less sensitive nerve endings than white people’ (Hoffman et al, 2016). If the very people being trained to treat patients harbour these beliefs then it is no surprise that black and other minority ethnic patients are less likely to be believed.
These are, no doubt, very hard problems to solve but we need solutions now to improve patient care for those who are most often left behind.
How can we help patients be heard better?
At The PSC, we’ve worked a lot in urgent care and with disorders that are prone to the problems described. For instance, Sickle Cell Disease (SCD) is a disorder that primarily affects black communities. These patients are susceptible to pain crises which can often end up with unsatisfactory trips to the emergency department. SCD patients are sometimes assumed to be associated with opioid abuse and addiction (Ruta et al. 2016), and so their requests for pain relief can be met with trepidation.
Through this work, here’s what we’ve learned about helping patients to be heard:
Care passports, maybe even electronic ones
Care passports have long been used to help patients with learning disabilities. They can be carried around and used to help explain underlying problems and past medical history to practitioners when an individual may struggle to explain this themselves. They represent a shortcut to help busy medical practitioners in non-elective settings and could be extended to patients that for other reasons may struggle to be believed or fully understood. Even better, growing interoperability capabilities could enable patient records to contain alerts of flags that bring important information to clinicians and minimize the burden on patients to explain their situations repeatedly.
Virtual Multi-Disciplinary Teams and specialist input
When living with a rare condition, patients aren’t always lucky enough to live close to a specialist. The rapid growth we’ve seen in virtual consultations presents a golden opportunity to expand access to experts. Whilst current commissioning is determined by geographical boundaries, we at The PSC can support specialist centres to expand their service reach and ensure access and funding to help patients further afield. This means that someone living in a remote area can access a Haematology specialist or Dermatologist with expertise in the skin of people of colour.
Patient training for advocacy
The NHS is increasingly stepping up its patient engagement approach, in important areas including patient co-design and even co-delivery. This is naturally one of the best ways to embed the patient voice in services, and to avoid some of the experiences described above.
In the interim, peer-led support groups can be a fantastic opportunity for patients to learn from each other, especially when it comes to sharing stories on how to advocate for oneself in healthcare settings.
This series aims to highlight major causes of inequality in healthcare and to start a conversation about approaches that could help move the dial towards a more equal and inclusive health and care system. If you have experiences in this area, then we’d love to hear from you at hello@thepsc.co.uk. We’ll be back with the next piece in this series very soon.
Authors: Katie Burns, Arup Nath
Latest News & Insights.

NHS Confed Expo 2026: Join our session
Joe Norbury will be joining system leaders at NHS Confed Expo to share practical…

The Next 20: Home First and the future of hospital discharge
Our latest episode of 'The Next 20' sees Chris Bradley speaks with Rachel Kemp…

The Next 20: The Analogue to Digital Shift
Digital transformation in healthcare is not just about technology. In this…

