26/02/2021
Strategy & Finance
NHS reforms pave the way to a more holistic approach to healthcare – but will they stick?
New proposals will see a greater focus on integrated care across the UK. The PSC’s strategy team explains how it could improve public health and the three factors that could see these reforms finally take hold.
On the 11th of February, The Department of Health and Social Care (DHSC) launched a blueprint for NHS and social care reform post-COVID. The proposals show a shift towards a more holistic, joined-up approach to healthcare that could improve population health, provide better care in the community, and ease pressure on hospitals.
The need for more integrated care has been highlighted by COVID-19 where health systems have had to adapt quickly to offer better community or at-home care. However, this is also representative of a long-term trend - our population is getting older and with this, more people have long-term health conditions that need regular management, which can often be done better outside of hospitals.
While integrated care is not a new concept, the reforms will see Integrated Care Systems (ICSs) finally gain legal recognition. Care can no longer be seen as something that simply takes place in hospitals, and now the winds may finally be blowing in the right direction to create positive long-term change.

Why is Integrated Care so important?
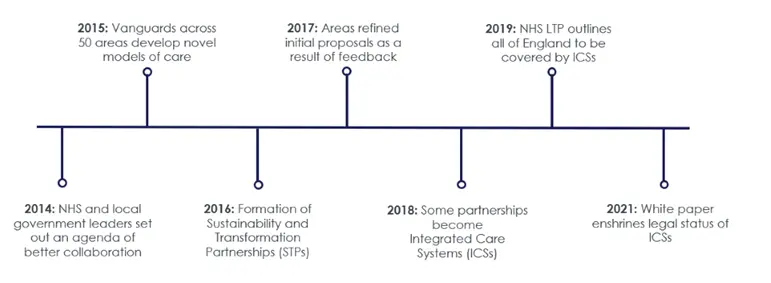
The legal recognition of ICSs marks a concrete step towards continued collective action, with the removal of internal legal restrictions and the establishment of a legal basis for decision making and governance. This is the latest in a series of moves towards integration since 2014 (see Figure 1).
The goal of an ICS is to maintain population health - ideally through prevention rather than treatment - with incentives and funding mirroring the DHSC’s aim to keep people out of hospital. The ICS reflects that leading a healthy life involves more than just treating physical ailments; it encompasses everything from having good living conditions to being supported by a community. The main three goals are:

ICSs are partnerships that bring together: NHS Acute, community and Mental Health Trusts; NHS commissioners (CCGs); local authorities; and other strategic partners including the voluntary, community, and social enterprise sectors.
Why could these reforms finally stick?
A transition to a more holistic approach to healthcare has the potential to improve outcomes for the whole population. Greater focus on prevention and community care can help prevent the worsening of conditions that would put people in hospital. In turn, this means more hospital resources are available to for those who need them most.
Changing the legal status of ICS’s is important but won’t create a set of thriving integrated systems alone. We believe however, that the following 3 factors mean that the most recent round of reforms will be successful in delivering integrated care:
- Covid-19 - the pandemic has transformed the delivery of care, with integration happening rapidly in response to the demand for alternative spaces of care. This precedent illustrates the capability for change.
- The direction of travel towards population health management – this major transition in healthcare acts as a catalyst for strategy development. ICS leaders will be able to formulate shared goals and collective aims around a clear ambition.
- Digital developments – digital capabilities are consistently improving, with the digital cornerstones of collaboration: data integration and system interoperability becoming increasingly viable. This allows for changes such as better virtual monitoring and assessment.
With these three factors coming together, the stage is set for the NHS to truly move towards a more integrated, holistic service. This will take huge changes in mindset, processes, and ways of working across the NHS and beyond, but the pay off could be enormous. We look forward to working with Trusts to make this happen.
Authors: Niamh Bridson Hubbard, Gideon Shapiro
Latest News & Insights.

The Next 20: Home First and the future of hospital discharge
Our latest episode of 'The Next 20' sees Chris Bradley speaks with Rachel Kemp…

The Next 20: The Analogue to Digital Shift
Digital transformation in healthcare is not just about technology. In this…

Our APPO Process: How to get real value from AI
AI is exciting, and experimenting with it is the right instinct. But, left…